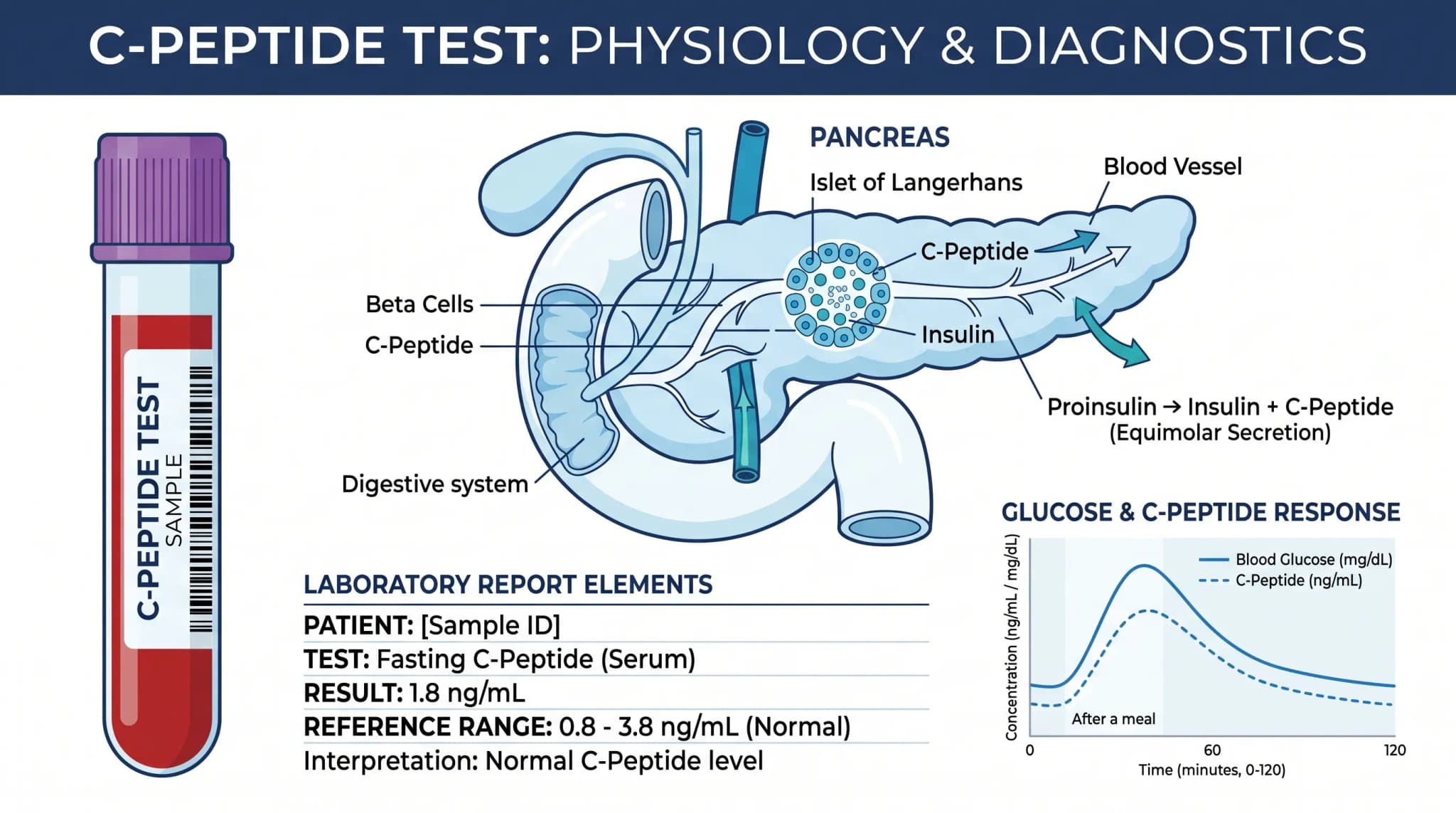
A C-peptide test measures a small peptide released when the pancreas makes insulin. Because insulin and C-peptide enter the bloodstream together, this assay helps show how much insulin the body produces on its own. In many settings, a C-peptide blood test or C peptide blood test gives a clearer picture of natural pancreatic output than an insulin-only result because C-peptide stays in the blood longer and does not reflect insulin that comes from outside the body.
This topic matters because the number does not describe glucose control by itself. Instead, the result adds context about beta-cell activity, which can support work on uncertain diabetes type, low blood sugar, or changes in pancreatic function over time. Therefore, a good C peptide test guide should explain what the lab measures, how sample timing changes interpretation, and why official reference ranges vary from one laboratory to another.
What C-peptide is and what the test measures
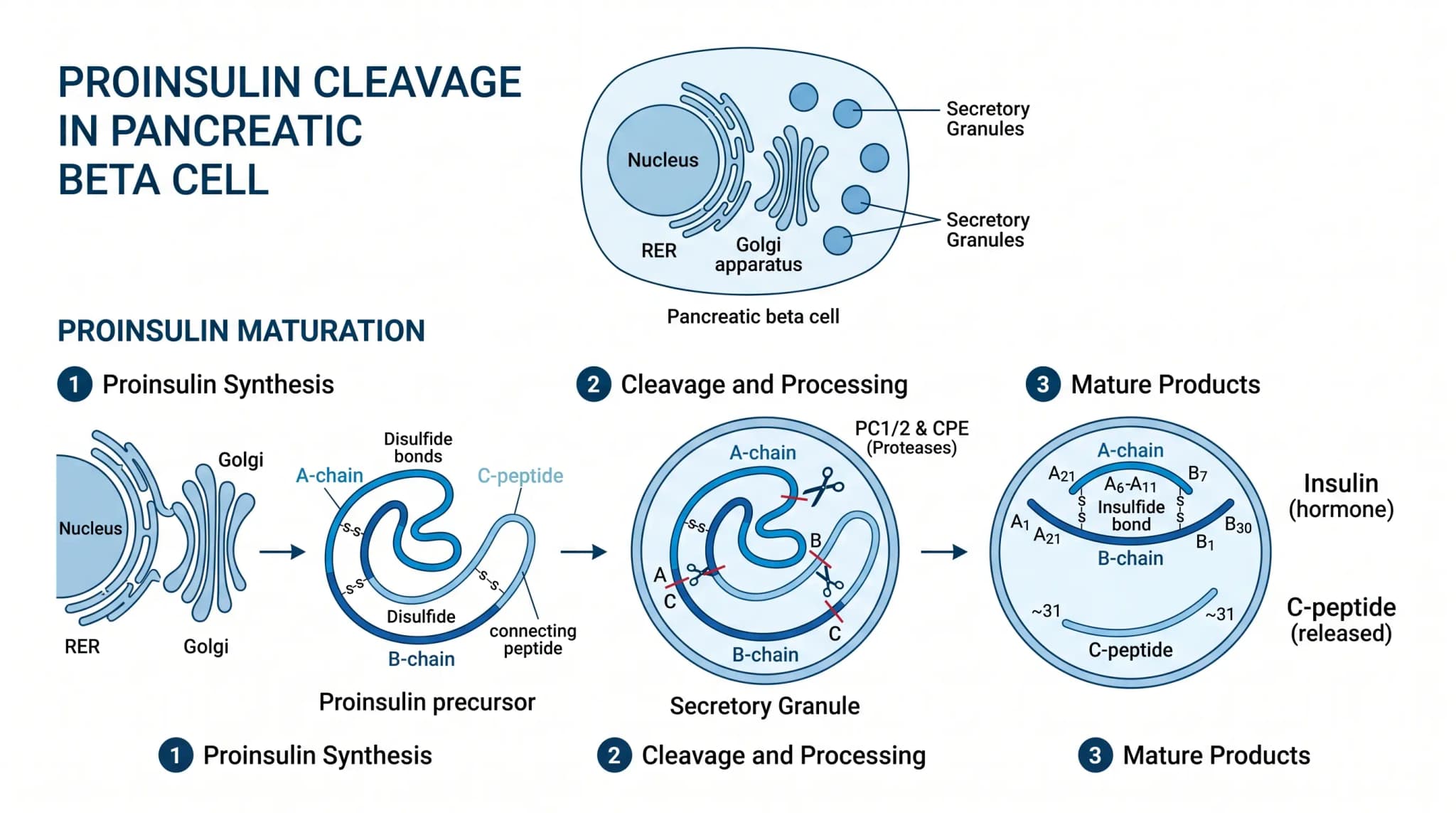
How C-peptide is linked to insulin production
The pancreas first makes proinsulin, then splits it into insulin and C-peptide before release. Because both parts enter the bloodstream together, the assay works as a marker of how much insulin the pancreas is making under that test condition. In addition, MedlinePlus and Labcorp note that insulin and C-peptide are released in equal amounts, while C-peptide remains in circulation longer, which helps a C-peptide blood test capture endogenous insulin output more steadily.
The easiest way to read this lab is simple. It is less about sugar itself and more about the pancreas behind the sugar result. A C peptide blood test does not measure glucose control directly. However, it can add useful context when glucose, A1c, insulin, and symptoms do not tell a complete story on their own.
Why C-peptide testing is different from insulin testing
An insulin result shows how much insulin is present in the sample. A C-peptide test, by contrast, focuses on insulin made by the pancreas, which makes the number easier to interpret when a person already uses insulin from outside the body. Because of that difference, MedlinePlus and UCSF both describe the assay as a way to separate natural insulin production from outside insulin exposure.
Another difference involves stability. C-peptide stays in the blood longer than insulin, so a C peptide test may reflect pancreatic output more consistently across short time windows. Moreover, Labcorp notes that insulin antibodies can interfere with insulin assays, while C-peptide can still help show residual beta-cell function.
Measure | Main question | What it reflects |
|---|---|---|
C-peptide | How much insulin the pancreas makes | Natural insulin production |
Insulin | How much insulin is present | Total insulin in the sample |
C-peptide with glucose context | How pancreatic output fits the glucose level | Beta-cell activity under that condition |
This quick comparison reflects how official sources describe the two measurements and why laboratories often read them together.
Why a C-peptide test may be ordered
Evaluating insulin production in diabetes
Care teams often order this assay when they need a better sense of ongoing insulin production in someone living with diabetes. MedlinePlus, UCSF, Quest, and RCPA all describe it as a tool for assessing pancreatic beta-cell function and for helping separate type 1 from type 2 diabetes in selected cases. As a result, the C-peptide test often appears when the diabetes label seems uncertain or when care planning depends on whether the pancreas still produces meaningful insulin.
That does not mean the assay replaces glucose-based diagnosis. MedlinePlus states clearly that laboratories use blood glucose and related tests to screen for and identify diabetes, while a C peptide test adds context about endogenous insulin output. Therefore, the result works best as one part of a broader lab picture.
Investigating low blood sugar or suspected insulinoma
This lab also plays an important role when low blood sugar needs more explanation. MedlinePlus says it can help find the cause of hypoglycemia, and Labcorp notes that the principal use of C-peptide is evaluation of hypoglycemia. For example, a high insulin result paired with a high C-peptide result suggests that the pancreas is producing that insulin, while a high insulin result paired with a low C-peptide result points in another direction.
The same logic explains why the C-peptide blood test can support work on suspected insulinoma, a pancreatic tumor linked with excess insulin output. MedlinePlus and Quest both list insulinoma-related evaluation as a common use of the assay. However, the number still needs glucose context and other lab data before anyone should draw broad conclusions.
When the assay is used
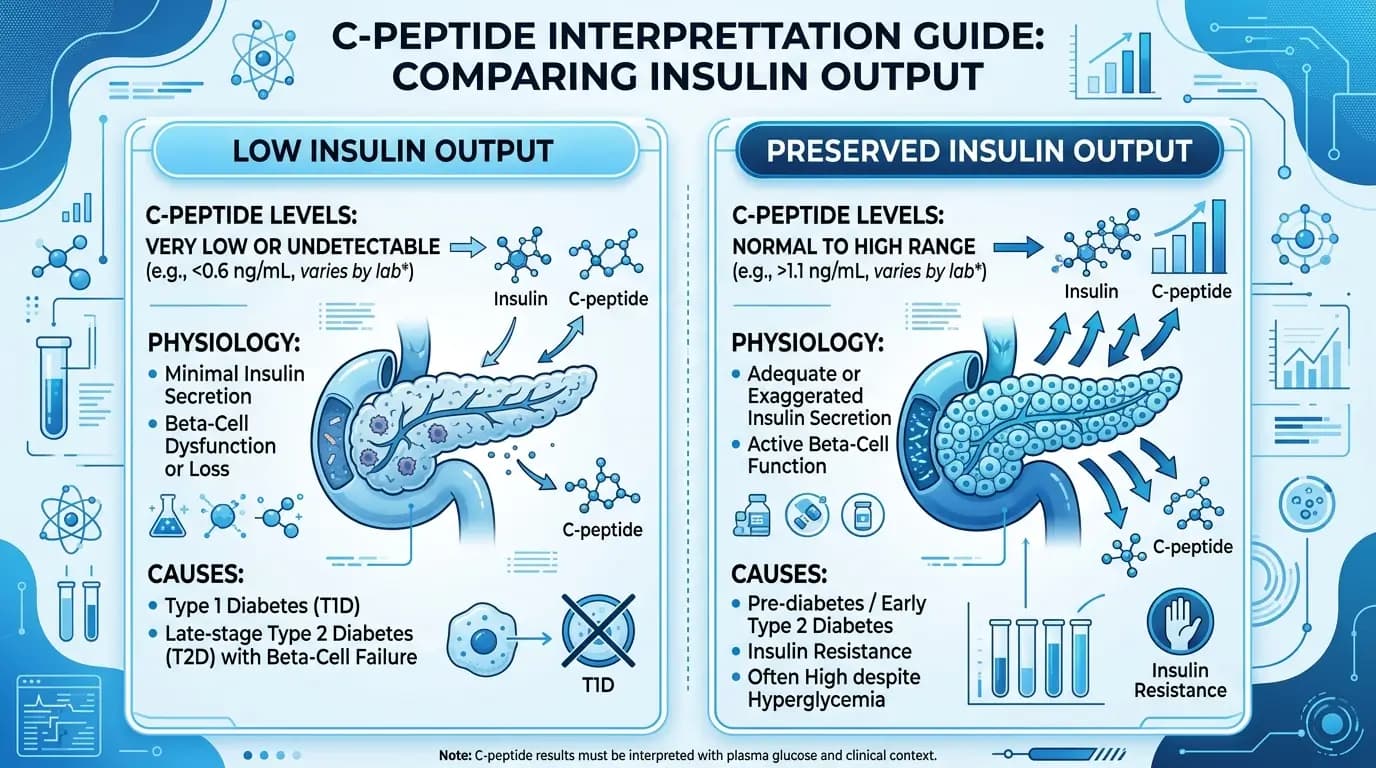
Distinguishing between type 1 and type 2 diabetes
When diabetes type is not obvious, this marker can add helpful evidence. MedlinePlus, Quest, and RCPA all state that it can help distinguish type 1 from type 2 diabetes by showing whether beta-cell insulin output is very low, preserved, or relatively high for the glucose level at the time of sampling. For that reason, a C peptide test often appears in cases that do not fit the most common pattern.
Even so, the result does not act like a standalone label. A low number may look different after fasting than after a meal, and a higher number may have different meaning when kidney function changes. Therefore, a C-peptide test supports classification, but it should stay tied to glucose, history, and the laboratory method used.
Monitoring pancreatic function and care planning
Beyond diabetes type, the assay can show whether pancreatic output appears stable, falling, or preserved over time. Quest and Labcorp describe it as useful for beta-cell function review and for certain transplant or pancreas-related follow-up settings. Because of that, a C peptide blood test may help frame longer-term discussions about insulin reserve rather than just one isolated lab moment.
Consistency matters here. RCPA notes that reference intervals are method dependent, and MedlinePlus says normal ranges can vary between laboratories. In other words, serial comparison works best when the same type of C-peptide blood test and the same laboratory method appear across repeated checks.
How the C-peptide test works
Blood and urine sample options
Most of the time, laboratories use blood. MedlinePlus says the assay usually uses a blood sample, although a 24-hour urine collection is another option. Labcorp adds that urine C-peptide can help when continuous assessment of beta-cell function is desired or when frequent blood sampling is not practical.
However, a C-peptide blood test remains the format most people mean when they talk about this topic. It is simpler for routine interpretation, and official pathology references list serum immunoassay as a standard specimen and method. Meanwhile, urine collection usually serves more specific situations that need a broader time window.
What happens during the procedure
For a blood sample, a health professional collects blood from a vein in the arm with a small needle. MedlinePlus says the draw usually takes less than five minutes, and UCSF notes that some people feel only a brief prick or sting, followed by minor soreness or bruising. So, from a practical standpoint, the C peptide test is a routine laboratory visit rather than a complex procedure.
For urine-based testing, the process lasts longer because the sample covers a full 24-hour collection period. MedlinePlus says the laboratory gives a container and instructions for collection and cold storage during that period. As a result, many people find the blood-based format easier unless the reason for testing favors urine.
How to prepare for a C-peptide test
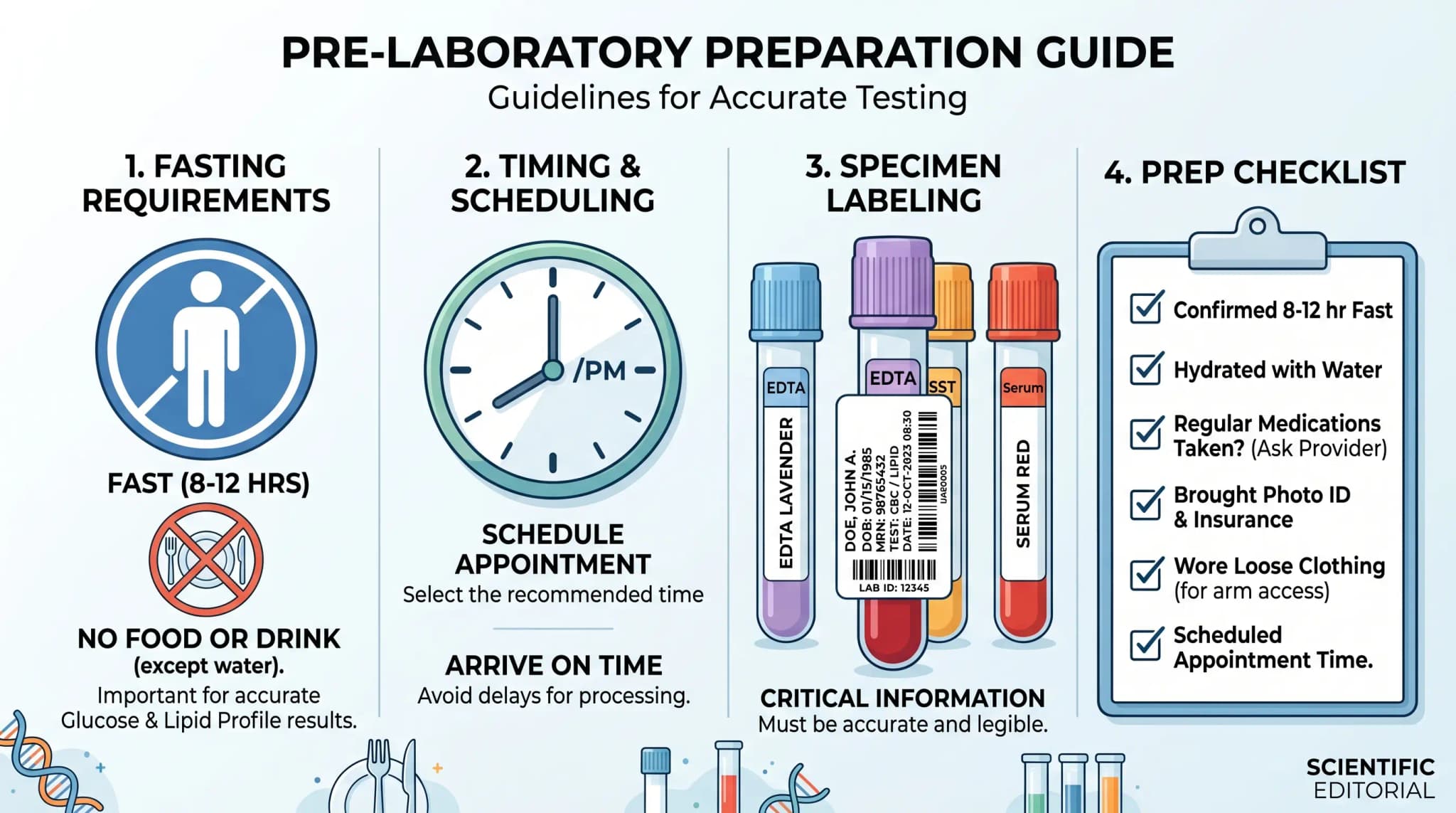
Fasting requirements and timing considerations
Preparation depends on the reason for testing. MedlinePlus says some people may need to fast for 8 to 12 hours before a C-peptide blood test, while Labcorp lists 14 to 16 hours for basal values in one fasting method. In addition, MedlinePlus notes that providers may also check the marker after food when they want to see how the pancreas responds under active stimulation.
This point is easy to miss, but it matters. A fasting C peptide test and a post-meal C peptide blood test do not answer exactly the same question, even when both measure the same analyte. Therefore, anyone reading the report should first ask under what conditions the sample was taken.
Factors that may affect the results
Several factors can shape how the result is read:
fasting versus post-meal timing
the glucose level at collection
kidney function
medications that may affect the result
assay method differences between laboratories
high biotin intake before sampling
MedlinePlus says medications can affect results, and Labcorp warns that high biotin intake may interfere with some related insulin and C-peptide assays, with a 72-hour pause recommended in that setting. RCPA also notes that intervals are method dependent, which means one report should be read against the range printed by that laboratory, not against a random range from elsewhere.
Kidney function deserves special attention. MedlinePlus lists kidney failure among causes of high C-peptide levels, and Labcorp notes that C-peptide can rise in renal failure. Because of this, a C-peptide test can look higher for reasons tied to clearance rather than production alone.
Understanding C-peptide test results
Normal C-peptide ranges
No single universal interval fits every report. UCSF lists a general blood reference interval of 0.3 to 3.3 ng/mL, while RCPA lists a fasting interval of 200 to 900 pmol/L and notes that the method matters. Labcorp also publishes a fasting interval of 1.1 to 4.4 ng/mL for one assay, and MedlinePlus says normal ranges can vary slightly among laboratories.
That variation does not mean the data are unreliable. Instead, it shows why a C peptide test must stay tied to the exact method, sample type, and timing. In summary, the best first step with any C-peptide blood test result is to read the reference range printed on that report and compare it with the glucose value collected at the same time.
What low and high C-peptide levels may indicate
A low result usually suggests low insulin production by the pancreas. MedlinePlus and UCSF both note that a low value may be normal after fasting or low blood sugar, yet it can be abnormal when blood sugar is high and the pancreas would be expected to release insulin. Because of that, a C-peptide test needs context before the number becomes meaningful.
A high result often points toward increased insulin production or slower clearance. MedlinePlus lists type 2 diabetes, insulinoma, kidney failure, and low potassium among common reasons for a higher value. Therefore, a C peptide blood test can raise useful questions, but it does not settle those questions on its own.
Risks, value, and limits of the test
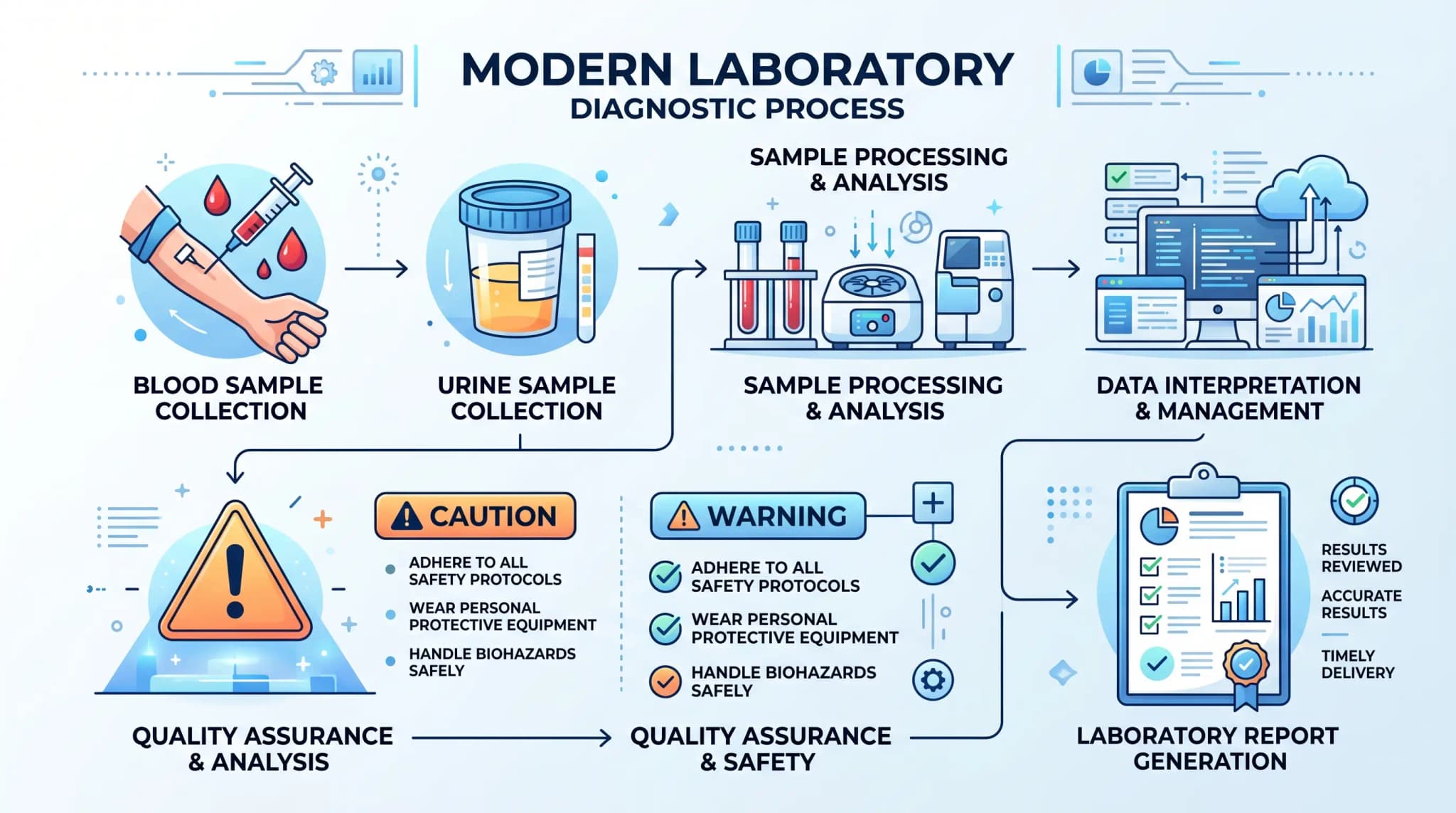
Possible risks of sample collection
This laboratory test carries very little risk when done with a blood draw. MedlinePlus says most people notice only slight pain, a small bruise, or short-lived soreness at the collection site. For urine collection, MedlinePlus reports no known risks.
Because the procedure is straightforward, most of the real challenge comes from timing and interpretation rather than sample collection itself. A fasting C-peptide blood test may require planning around meals, while a urine-based check asks for careful collection across the full 24-hour period.
Why the test is useful and where interpretation can vary
The strongest value of this assay is its ability to reflect pancreatic insulin production more directly than an insulin result alone in many real-world settings. MedlinePlus, UCSF, Quest, and Labcorp all point to that role when diabetes type is uncertain, when hypoglycemia needs explanation, or when beta-cell function needs closer review. In addition, Labcorp notes that C-peptide stays informative when insulin antibodies complicate some insulin assays.
Its main limit is context. A C peptide test does not diagnose diabetes by itself, and a C-peptide blood test without glucose, timing, kidney function, or method details can be hard to read correctly. Overall, the assay is most powerful when it sits inside a full lab picture rather than acting as a standalone answer.
C-peptide test and peptide researches
How peptide researches supports research-focused education and quality standards
A research-focused article on this topic should stay educational, careful, and specific. That means explaining what the analyte is, how a C-peptide test fits into laboratory interpretation, and why a C peptide blood test needs sample context. It also means avoiding exaggerated claims, personal-use framing, or language that turns a lab topic into a product promise.
For Peptide Researches, the stronger approach is to present peptide information as a laboratory education resource. In detail, that includes clear naming, batch-level identity and purity documentation where relevant, neutral descriptions of handling and storage, and a visible statement that products are for laboratory research use only and not intended for use in humans or animals. Likewise, educational pages can discuss the C peptide test in a research-aware tone without drifting into unsupported outcome claims.
Conclusion
A C-peptide test helps show how much insulin the pancreas makes under a specific set of conditions. A C peptide test can support work on diabetes classification, hypoglycemia evaluation, and longer-term beta-cell review, while a C-peptide blood test can add detail that an insulin-only result may miss. Overall, the most accurate reading comes from matching the number to glucose, timing, kidney function, and the laboratory method rather than reading the result in isolation.