A B-Type Natriuretic Peptide (BNP) test is a blood test that measures a heart-related biomarker linked to pressure and stretch inside the heart. Clinicians often use it when a person has shortness of breath, swelling, or other signs that could point to heart failure and usually interpret it together with symptoms, exam findings, and other heart tests.
BNP belongs to a group of signaling molecules called natriuretic peptides. Because I wrote this article for beginners and research-minded readers, I explain what the BNP test measures, when clinicians use it, what the results can and cannot show, and how a lab-focused website can discuss the topic clearly.
What a BNP test measures
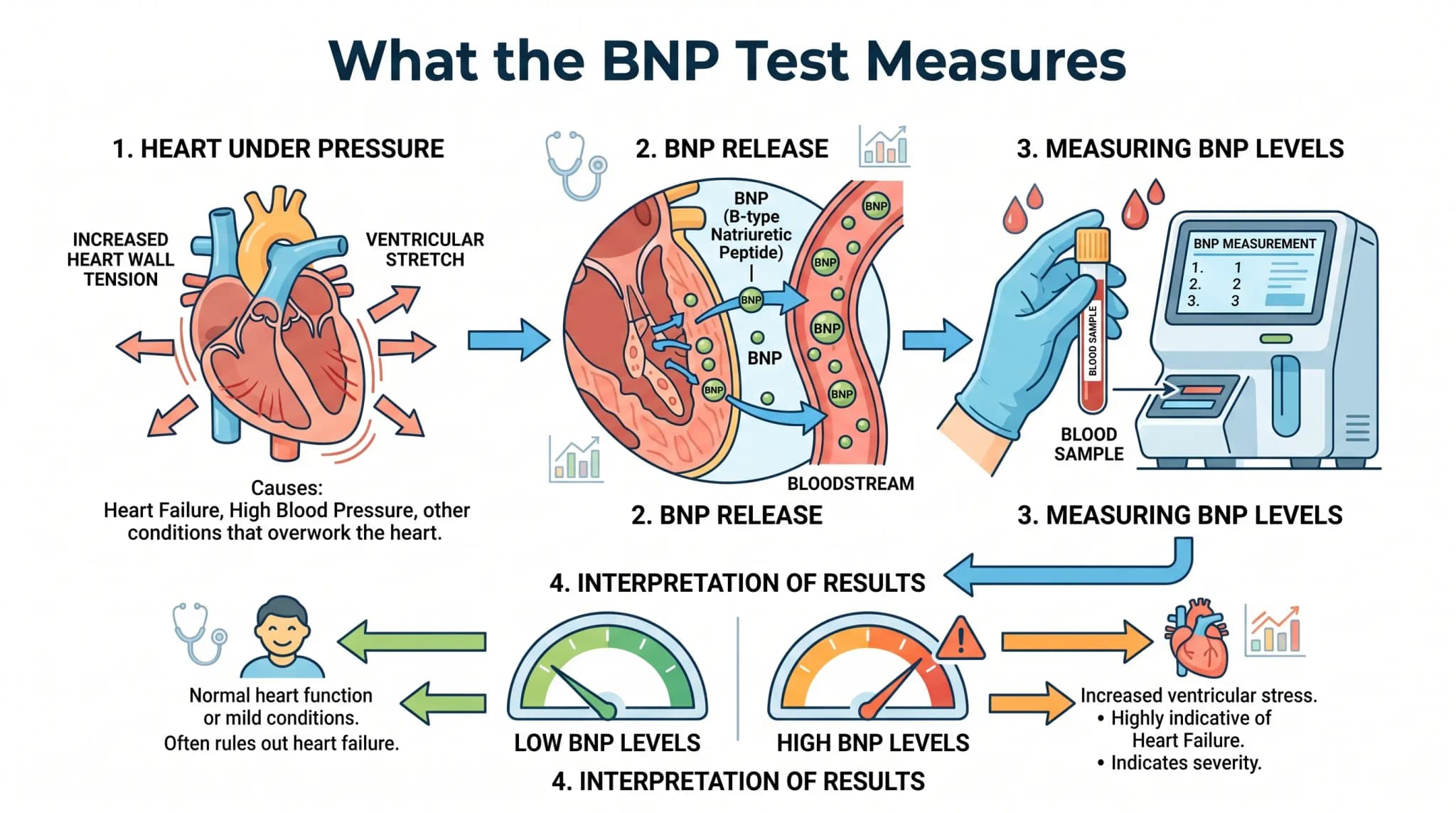
What BNP is and why the body releases it
The heart releases larger amounts of BNP when it is under greater pressure and has to work harder. In general, this happens when the chambers of the heart stretch. BNP then signals the blood vessels to widen and supports the removal of salt and water, which lowers workload on the heart.
That is why the BNP test is useful as a biomarker rather than as a standalone answer. A higher BNP value can suggest that the heart is under strain. However, the number does not explain the whole story by itself, because several other heart, lung, and kidney conditions can affect the reading as well.
Another helpful way to think about the BNP test is that it reflects hemodynamic stress rather than a single disease label. In other words, the assay is measuring the heart’s response to pressure and volume load. Because of that, the BNP test is most informative when the question is, “Is the heart under unusual strain right now, and how strongly does the biomarker support that concern?”
The difference between BNP and NT-proBNP
BNP and NT-proBNP come from the same precursor molecule, and clinicians use both for heart evaluation. MedlinePlus notes that the body uses NT-proBNP to make BNP, while heart strain can increase the release of both markers.
In practice, many labs measure either BNP or NT-proBNP rather than both at the same time. The two tests serve a similar purpose, yet their reference ranges are different. For that reason, readers should avoid comparing the number from one assay directly with the number from the other.
Marker | What it reflects | Common reporting pattern |
|---|---|---|
BNP | Active natriuretic peptide released with cardiac stretch | Often reported with a general reference point below 100 pg/mL |
NT-proBNP | Inactive fragment linked to BNP release | Often reported with age-related reference points |
The table above is a simplified comparison. Labs may use different methods, units, and reference intervals, so the report should always be read in the context of the assay that produced it.
Why a BNP test may be ordered
Symptoms and situations that can lead to testing
Doctors commonly request a BNP test when a person has symptoms that could reflect heart failure, especially when the cause of those symptoms is not yet clear. MedlinePlus and Testing.com both highlight shortness of breath as one of the most common reasons for ordering the test. Swelling, fatigue, cough, difficulty lying flat, and nighttime urination may raise the same question.
Common reasons a BNP test enters the picture include:
shortness of breath
swelling in the legs, ankles, abdomen, or neck veins
fatigue or general weakness
cough
trouble sleeping flat
a need to sort out whether symptoms are more likely heart-related or linked to another cause
Because many of these symptoms overlap with lung, kidney, and other conditions, clinicians value the BNP test as one piece of a broader workup instead of a final answer on its own.
This overlap explains why clinicians often pair the BNP test with a symptom review rather than use it as a broad screening tool for everyone. For example, unexplained breathlessness in the emergency room is a very different setting from a routine lab panel. Accordingly, the meaning of the BNP test depends not only on the number itself, but also on why the clinician ordered the test in the first place.
The role of BNP in evaluating possible heart failure
The BNP test plays an important role when heart failure is being considered. According to MedlinePlus, normal BNP or NT-proBNP levels in a person with shortness of breath can often help rule out heart failure, while high levels usually lead to more testing to confirm the cause.
At the same time, the test is not perfectly specific. A high value can support concern about heart failure, but it does not prove that diagnosis by itself. Therefore, BNP is best understood as a strong signal that helps direct the next step in evaluation.
When the BNP test is used in diagnosis and follow-up
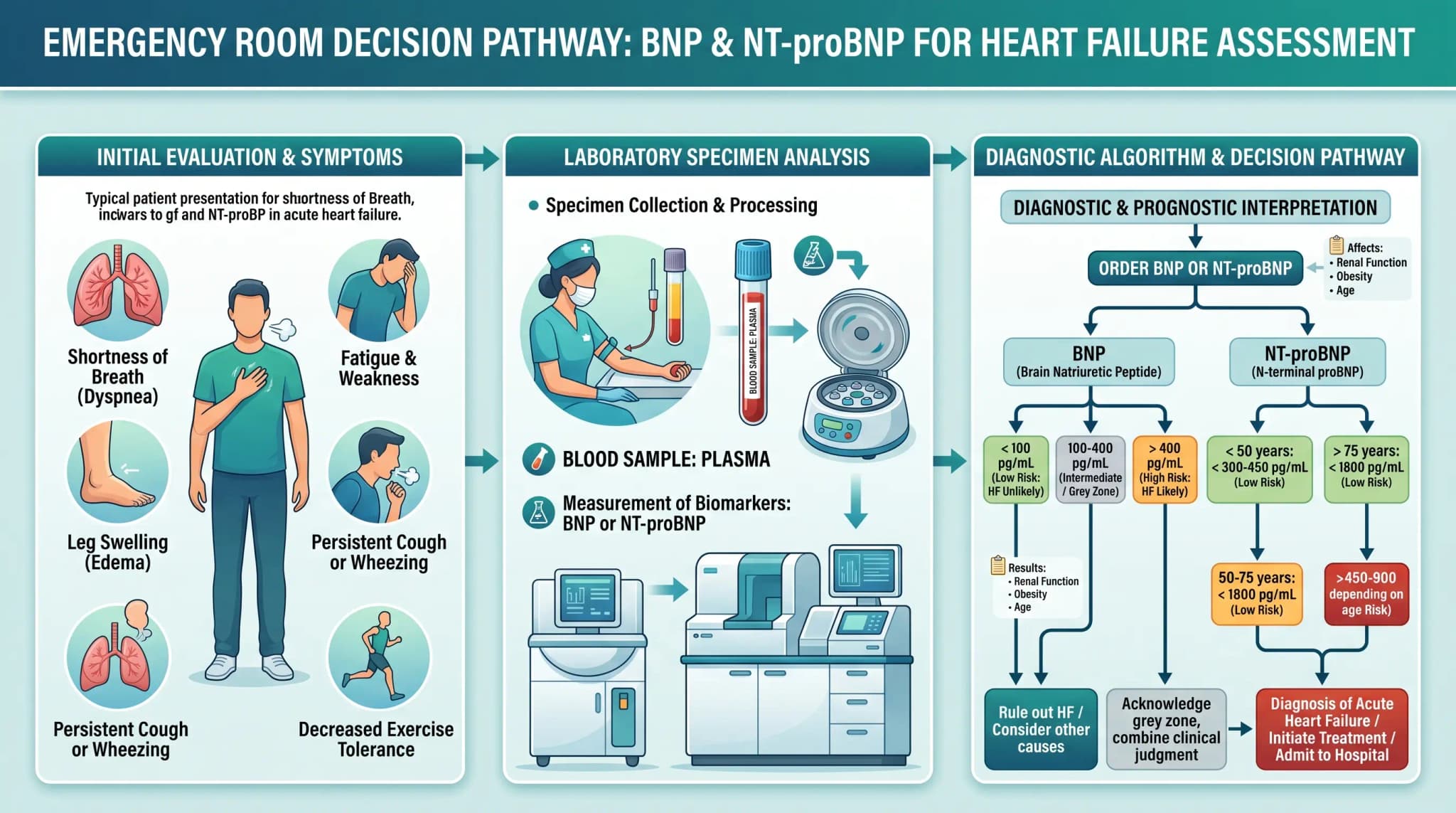
Use in people with shortness of breath
When someone arrives with unexplained shortness of breath, doctors often use the BNP test early because the result can help separate heart-related strain from other causes. The American College of Cardiology summarizes evidence showing that, in emergency settings, BNP performs well in people presenting with shortness of breath, especially around the commonly used 100 pg/mL cutoff.
Even so, interpretation still depends on context. A normal value can be very reassuring, yet it is not perfect in every situation. MSD Manual notes that normal BNP levels do not fully exclude heart failure, particularly in people with obesity or heart failure with preserved ejection fraction (HFpEF).
Use in ongoing monitoring of chronic heart failure
Once clinicians have already identified heart failure, they may use BNP or NT-proBNP again to learn whether symptoms are worsening or whether the overall picture is becoming more serious. MedlinePlus states that healthcare providers can use these tests to check if an increase in symptoms means the condition has gotten worse and to estimate the chance of further decline.
However, clinicians should still interpret serial BNP testing alongside the wider clinical picture, including symptoms, kidney function, imaging, and physical findings. In other words, follow-up numbers provide information, but they do not replace full reassessment.
How the BNP test works
Sample collection and test procedure
A BNP test usually starts with a routine blood draw from a vein in the arm. MedlinePlus explains that a healthcare professional collects the sample with a small needle into a tube or vial, and the process usually takes less than five minutes. In some hospital settings, clinicians can use a fingerstick method for faster turnaround.
The process is simple from the reader’s point of view, but the lab side matters too. After collection, the laboratory analyzes the sample for BNP or NT-proBNP concentration and matches the final report to the method and reference interval it uses. That is why different platforms should not be treated as interchangeable without context.
Preparation before the test
Most sources state that no special preparation is needed for a BNP test. Testing.com and MedlinePlus both note that fasting or other major prep steps are generally not required.
Still, local instructions matter. In addition, the care team may review the full context of symptoms, current health status, and other recent tests when deciding how to interpret the result.
Understanding BNP test results
Normal ranges and common cutoff points
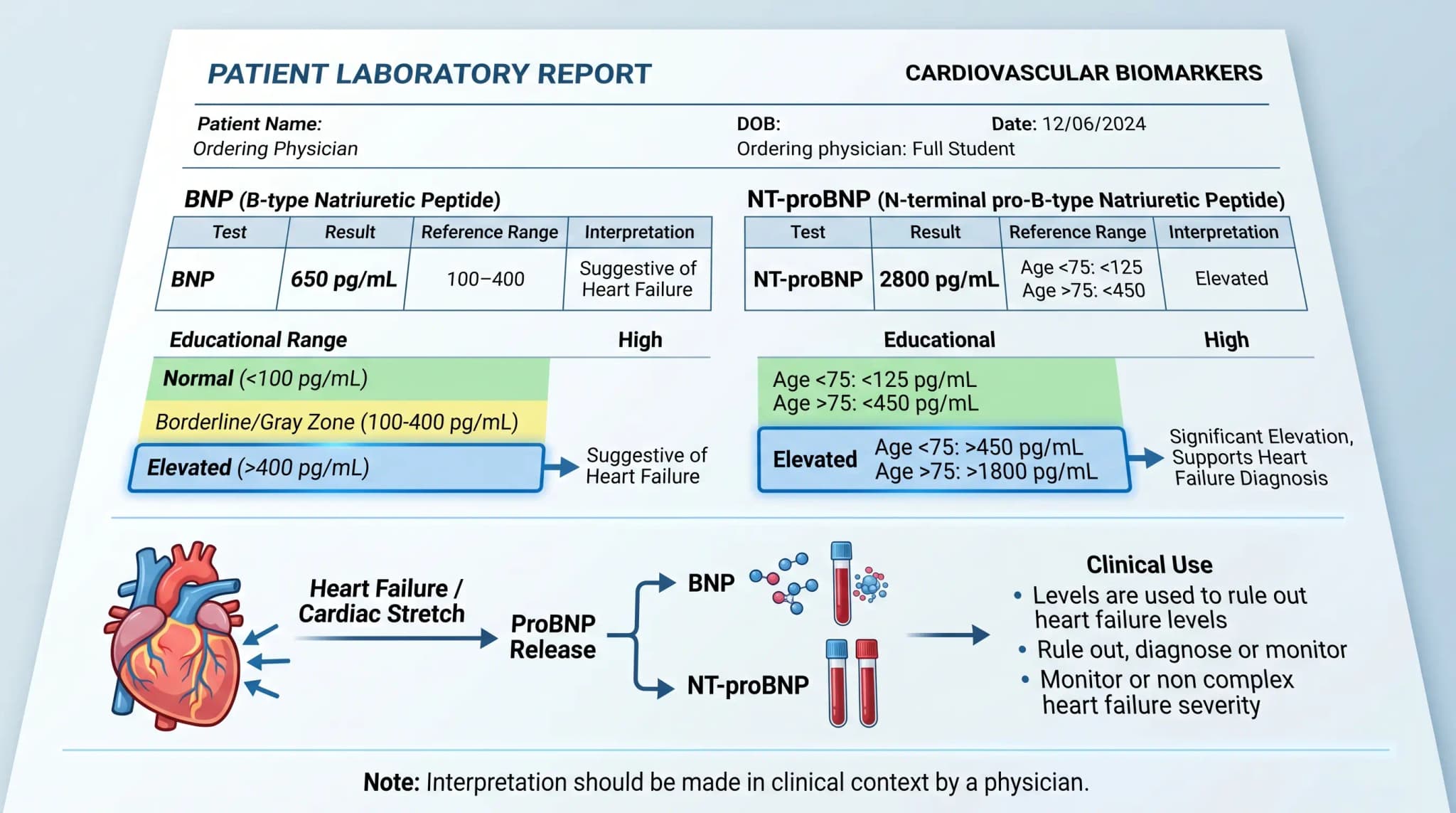
A normal BNP value is often described as less than 100 pg/mL. Cleveland Clinic lists that general reference point, and MedlinePlus notes that values below 100 pg/mL may suggest heart failure is less likely, although exact ranges can vary by lab.
For NT-proBNP, the picture is different because age-related cutoffs are often used. Cleveland Clinic lists general normal values below 125 pg/mL for people under 75 and below 450 pg/mL for people over 75, while the American College of Cardiology highlights age-related rule-in cutoffs of 450 pg/mL for those under 50, 900 pg/mL for ages 50 to 75, and 1800 pg/mL for those over 75 in acute settings.
These numbers are helpful, but they are not universal rules. Reference intervals can differ by laboratory, by assay design, and by the question being asked, such as rapid triage versus longer-term follow-up. For that reason, the most useful reading is the one tied to the specific report in front of you.
Reports may show the result in pg/mL, ng/L, or occasionally other units depending on the reporting system. Meanwhile, the reference interval printed on the report matters as much as the number itself. A BNP test result without its unit, method, or lab range is incomplete from an interpretation standpoint.
Factors that can affect interpretation
Several factors can shift BNP or NT-proBNP values even before heart structure is discussed. Cleveland Clinic notes that obesity can lower BNP levels. Testing.com adds that age, sex, body weight, and genetics can influence interpretation, while kidney disease and some lung conditions can raise values.
This is one of the biggest reasons the BNP test should never be read in isolation. For example, obesity may lower BNP levels despite real heart strain, while kidney dysfunction can push the number upward for reasons beyond heart failure.
Accuracy, limitations, and related tests
When BNP results may be less specific
The BNP test is useful, but it is not perfectly specific for heart failure. Testing.com notes that kidney failure, cardiomyopathy, pulmonary hypertension, sepsis, and other forms of heart disease can elevate BNP or NT-proBNP. Likewise, Cleveland Clinic lists chronic kidney disease, other heart disease, and certain lung conditions among other reasons for a higher result.
On the other hand, a lower value does not always close the case. MSD Manual points out that BNP can be lower in obesity and that normal values do not fully exclude HFpEF. As a result, the BNP test works best as a decision-support marker rather than a yes-or-no answer.
This matters especially in gray-zone cases. A moderately elevated BNP test result may raise concern, but clinicians must still weigh it against age, kidney function, body size, rhythm status, and imaging findings. Conversely, a lower BNP test result may look reassuring, yet it does not automatically close the door on heart failure in every person or every subtype.
Other tests often used alongside BNP
The American Heart Association notes that natriuretic peptides are usually part of a larger heart workup that may include electrolyte testing, albumin, and creatinine. Cleveland Clinic also notes that doctors may order an electrocardiogram after an abnormal BNP result.
In real-world care, clinicians commonly interpret BNP together with imaging and rhythm evaluation. That may include an electrocardiogram, echocardiography, chest imaging, or other blood tests, depending on the symptoms and the suspected cause. Therefore, the most accurate understanding comes from combining biomarkers with structure, function, and symptom context.
Risks, value, and next steps
Possible risks and complications of the test
The BNP test carries very little risk because it is generally a routine blood draw. MedlinePlus says the most common issues are slight pain or bruising where the needle entered, and Testing.com lists rare problems such as lightheadedness, infection, or more noticeable bleeding.
Compared with imaging or invasive heart procedures, this makes BNP an accessible first-line biomarker in many settings. In particular, it can deliver useful information quickly when symptoms such as shortness of breath need fast sorting.
What happens after you receive the results
After you report the result, the next step depends on the full picture. High BNP or NT-proBNP values usually lead to more testing to confirm whether heart failure is present, while lower values may shift attention toward other explanations for symptoms.
Timing can vary. Cleveland Clinic says results may be available right away in emergency settings, often in under 15 minutes, while Testing.com notes that routine blood-draw results may take from hours to a few days depending on the method and setting.
BNP test and peptide researches

How peptide researches supports lab-focused education and research quality standards
A BNP test article on a research-focused peptide site should stay educational and lab-centered. Peptide Researches can use this topic to explain peptide-based biomarkers, assay language, reference ranges, and source transparency without turning the page into personal-use guidance. That approach fits a catalog-plus-education model better than promotional health language.
In practice, good research-quality communication means explaining what the biomarker is, clarifying what the assay can and cannot show, citing reliable sources, and separating educational content from any product catalog content. It also means using careful wording, because a biomarker article should inform readers about terminology and measurement rather than promise outcomes for any person or condition.
For a research-focused audience, this section matters because it shows how peptide terminology intersects with assay literacy. BNP is a peptide biomarker, yet a page about the BNP test should not blur the line between laboratory education and product language. Instead, a strong article explains the marker, the test context, the limits of interpretation, and the value of clear source documentation.
Conclusion
The BNP test is one of the most useful heart-related biomarker tests because it can add fast context when shortness of breath, swelling, or suspected heart strain need explanation. However, the number is most informative when it is read beside symptoms, age, body composition, kidney function, and other heart tests.
For beginners, the key takeaway is simple: BNP and NT-proBNP are not standalone verdicts. Instead, they are part of a broader interpretation process that helps sort out whether heart failure is likely, how serious it may be, and what additional evaluation may be needed. For researchers and lab-focused readers, the equally important point is assay context, because method, cutoff selection, and reporting format all shape what the final number means.